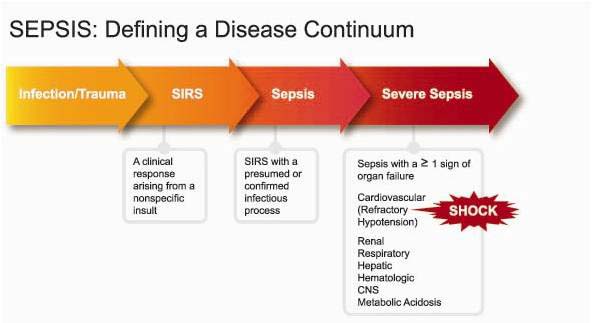
Seeking earlier recognition and treatment of hospital patients, Pitt researchers joined an international task force in January 2014 to redefine sepsis, a disease where the immune system damages its own organs and tissues in response to infection.
After analyzing 800,000 hospital records, the task force presented its results at a Critical Care conference in Orlando, Florida, on Feb. 20-24, and the researchers published their results in the Journal of the American Medical Association in February. In May, the researchers will publish the results in the the New England Journal of Medicine.
The task force worked to clarify the definition of sepsis and its criteria, which was last revised in 2001, according to Christopher W. Seymour, a member of the task force and assistant professor in Pitt School of Medicine’s Department of Critical Care Medicine and Emergency Medicine.
For Derek C. Angus, task force member and chair of Pitt’s Department of Critical Care Medicine, the goal was to use data analysis rather than opinions from a panel of experts to redefine sepsis. The data analysis is objective, whereas opinions from experts are subjective and variable, Angus said.
The task force analyzed medical records at 177 hospitals around the world to develop the new criteria, known as the quick Sepsis-related Organ Failure Assessment, or qSOFA.
The qSOFA criteria uses vital signs, such as altered mental status, low blood pressure and a faster respiratory rate, as opposed to blood work, to identify the disease faster.
According to the Centers for Disease Control and Prevention, sepsis kills more than 258,000 Americans each year and is the ninth leading cause of disease-related deaths.
“Infection is a common syndrome, but we don’t all get sick when a bacteria or virus invades the body. Some of us are at more risk, especially as we get older, the immune response gets dysregulated and an attempt to fight off infection can damage the kidneys or brain,” Seymour said.
Seymour said sepsis occurs in about two million patients every year and despite treatments, about one in 10 patients do not survive.
“About eight of 10 patients [in general] get sepsis within the first 48 hours of admission [to a hospital unit] so it was community acquired and the minority, the other two of 10, get infected in the hospital,” Seymour said.
Seymour said the criteria does not change the treatment method, which consists of antibiotics targeting the infected organism and site and, if needed, intravenous fluids.
Seymour said next step in treating sepsis is for hospitals to use the qSOFA test and analyze how early physicians recognize risk factors and when they begin treatment.
Currently, each hospital has its own protocol for identifying sepsis. Angus said the task force hopes hospitals around the world will utilize sepsis’ redefinition, creating a more standard evaluation method for patients in studies and scientific papers across several different languages.
Grants from the Society of Critical Care Medicine and the European Society of Intensive Care Medicine, the National Institute of General Medical Sciences and the National Heart, Lung, and Blood Institute funded the study.
The task force has redefined the condition, but the new meaning is only beginning to emerge in clinical settings such as hospitals and physician’s offices.
“It is sparking a huge debate. It is one of the most viewed papers on [the Journal of the American Medical Association], and is going to lead to a new discussion,” Seymour said.
The American College of Chest Physicians, the American College of Emergency Physicians and the Latin American Sepsis Institute refused to endorse the new definition because the task force did not include researchers from low and middle income countries, which have different experiences with sepsis, and because the new criteria will focus more specifically on a severely ill population.
Angus said the paper was downloaded 350,000 times from the Journal of the American Medical Association within the first 72 hours.
“Everyone with a database is probably trying to repeat what we already found,” Angus said. “There is a high-level of interest worldwide.”